Understanding Melasma – A Multifactorial Challenge
Melasma is a chronic hyperpigmentation disorder that presents as symmetric brown‑to‑gray‑brown patches on sun‑exposed facial areas—most often the cheeks, forehead, nose, and upper lip. The lesions may be epidermal, dermal, or mixed, which influences treatment response.
Key triggers are hormonal, genetic, and environmental. Fluctuations in estrogen and progesterone—seen during pregnancy, oral‑contraceptive use, or hormone‑replacement therapy—stimulate melanocyte activity. A hereditary predisposition and certain medications that increase photosensitivity also raise risk. UV radiation is a well‑established driver, but high‑energy visible light (HEVL) and long‑wave UVA further amplify melanogenesis, especially in Fitzpatrick skin types III‑VI.
Because light exposure is central to disease perpetuation, photoprotection is the cornerstone of any management plan. Broad‑spectrum sunscreens with SPF 30‑50 that block UVB, UVA, and VL (ide‑oxide‑tinted formulas) should be applied daily, reapplied every two hours, and complemented by protective clothing and wide‑brimmed hats. Consistent, high‑quality photoprotection not only prevents new pigment formation but also enhances the efficacy of topical and procedural therapies, forming the foundation for a personalized, long‑term melasma strategy.
Pathogenesis and Key Triggers of Melasma
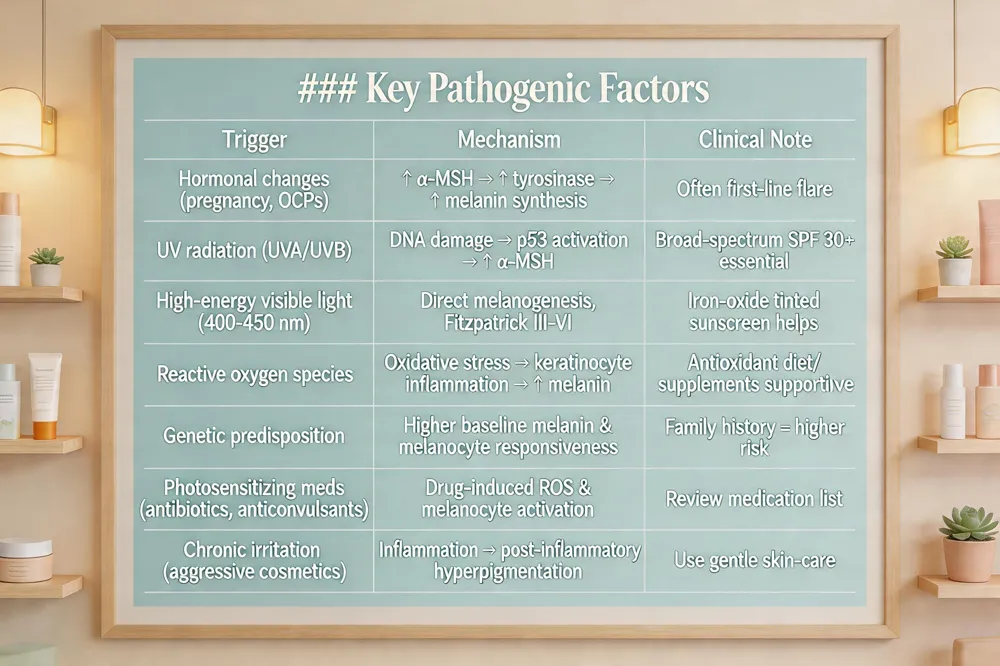
Key Pathogenic Factors
| Trigger | Mechanism | Clinical Note |
|---|---|---|
| Hormonal changes (pregnancy, OCPs) | ↑ α‑MSH → ↑ tyrosinase → ↑ melanin synthesis | Often first‑line flare |
| UV radiation (UVA/UVB) | DNA damage → p53 activation → ↑ α‑MSH | Broad‑spectrum SPF 30+ essential |
| High‑energy visible light (blue light 400‑450 nm) | Direct melanogenesis, especially in Fitzpatrick III‑VI | Iron‑oxide tinted sunscreen helps |
| Reactive oxygen species | Oxidative stress → keratinocyte inflammation → ↑ melanin | Antioxidant diet/supplements supportive |
| Genetic predisposition | Higher baseline melanin & melanocyte responsiveness | Family history = higher risk |
| Photosensitizing meds (antibiotics, anticonvulsants) | Drug‑induced ROS & melanocyte activation | Review medication list |
| Chronic irritation (aggressive cosmetics) | Inflammation → post‑inflammatory hyperpigmentation | Use gentle skin‑care |
 Melasma is a multifactorial hyperpigmentation disorder that most often Melasma appears as brown or gray‑brown patches on the cheeks, forehead, nose, and upper lip. Its development is driven primarily by Hormonal changes, such as pregnancy or oral contraceptive use, are major triggers for melasma, which stimulate melanocyte activity and increase melanin synthesis. UV radiation is a primary exacerbating factor; daily broad‑spectrum sunscreen (SPF 30+) is essential penetrates the epidermis, activating the p53 pathway and α‑MSH production, while high‑energy visible light (blue light, 400‑450 nm) also triggers melanogenesis, particularly in Fitzpatrick skin types III‑VI. Both UV and visible light generate reactive oxygen species that inflame keratinocytes, further amplifying pigment production and promoting Melasma often involves both the epidermis and dermis, making it more treatment to treatment. Genetic predisposition and photosensitizing medications (e.g., certain antibiotics and anticonvulsants) can contribute to melasma development, as families with a history of melasma often display higher baseline melanin levels and heightened melanocyte responsiveness. Certain medications—such as photosensitizing medications (e.g., certain antibiotics and anticonvulsants), antiepileptics, and some hormonal agents—can exacerbate the condition, as can chronic skin irritation from aggressive cosmetics or procedures. Consistent, Broad‑spectrum sunscreen (SPF 30 +, UV‑PF ≥ 20, preferably tinted with iron oxides) is essential to block UV and visible light, reduce oxidative stress, and prevent the cycle of pigment accentuation.
Melasma is a multifactorial hyperpigmentation disorder that most often Melasma appears as brown or gray‑brown patches on the cheeks, forehead, nose, and upper lip. Its development is driven primarily by Hormonal changes, such as pregnancy or oral contraceptive use, are major triggers for melasma, which stimulate melanocyte activity and increase melanin synthesis. UV radiation is a primary exacerbating factor; daily broad‑spectrum sunscreen (SPF 30+) is essential penetrates the epidermis, activating the p53 pathway and α‑MSH production, while high‑energy visible light (blue light, 400‑450 nm) also triggers melanogenesis, particularly in Fitzpatrick skin types III‑VI. Both UV and visible light generate reactive oxygen species that inflame keratinocytes, further amplifying pigment production and promoting Melasma often involves both the epidermis and dermis, making it more treatment to treatment. Genetic predisposition and photosensitizing medications (e.g., certain antibiotics and anticonvulsants) can contribute to melasma development, as families with a history of melasma often display higher baseline melanin levels and heightened melanocyte responsiveness. Certain medications—such as photosensitizing medications (e.g., certain antibiotics and anticonvulsants), antiepileptics, and some hormonal agents—can exacerbate the condition, as can chronic skin irritation from aggressive cosmetics or procedures. Consistent, Broad‑spectrum sunscreen (SPF 30 +, UV‑PF ≥ 20, preferably tinted with iron oxides) is essential to block UV and visible light, reduce oxidative stress, and prevent the cycle of pigment accentuation.
First‑Line Topical Therapy and Prescription Creams
First‑Line Prescription Regimens
| Agent | Typical Concentration | Primary Action | Common Combination |
|---|---|---|---|
| Hydroquinone | 2‑4 % | Tyrosinase inhibitor | Triple‑combo (hydroquinone + tretinoin + low‑potency steroid) |
| Retinoid (tretinoin) | 0.025‑0.05 % | Increases epidermal turnover | Paired with hydroquinone |
| Mild corticosteroid | Hydrocortisone 1 % | Reduces retinoid irritation | Part of triple‑combo |
| Azelaic acid | 15‑20 % | Anti‑inflammatory, tyrosinase inhibition | Alternative to hydroquinone |
| Tranexamic acid (topical) | 2‑5 % | Inhibits melanocyte‑vascular cross‑talk | Adjunct to hydroquinone |
| Kojic acid | 1‑2 % | Tyrosinase inhibition | Add‑on for mild cases |
| Niacinamide | 5 % | Improves barrier, reduces inflammation | Can be layered under sunscreen |
Application tip: Apply evening, start every every alternate days to assess tolerance, then increase to once/twice daily.
 Melasma is best managed initially with prescription‑strength depigmenting creams. The gold‑standard agent is hydroquinone (2‑4 %); most clinicians combine it with a retinoid and a mild corticosteroid in the classic “triple‑combo” (hydroquinone + tretinoin + low‑potency steroid). This regimen accelerates melanin inhibition, promotes epidermal turnover, and reduces inflammation, while the steroid mitigates retinoid‑related irritation. For patients who cannot tolerate hydroquinone, gentler alternatives such as azelaic acid (15‑20 %), topical tranexamic acid (2‑5 %), kojic acid, or niacinamide provide meaningful brightening with a lower risk of dermatitis.
Melasma is best managed initially with prescription‑strength depigmenting creams. The gold‑standard agent is hydroquinone (2‑4 %); most clinicians combine it with a retinoid and a mild corticosteroid in the classic “triple‑combo” (hydroquinone + tretinoin + low‑potency steroid). This regimen accelerates melanin inhibition, promotes epidermal turnover, and reduces inflammation, while the steroid mitigates retinoid‑related irritation. For patients who cannot tolerate hydroquinone, gentler alternatives such as azelaic acid (15‑20 %), topical tranexamic acid (2‑5 %), kojic acid, or niacinamide provide meaningful brightening with a lower risk of dermatitis.
What are the best treatments for melasma on the face?
First‑line therapy is a triple‑combo cream or hydroquinone monotherapy, applied once or twice daily. Adjunctive agents—azelaic acid, tranexamic acid, vitamin C, or niacinamide—can be layered to enhance results. For resistant lesions, in‑office chemical peels (glycolic, lactic, low‑strength TCA) or light‑based modalities (low‑fluence Q‑switched Nd:YAG, IPL, non‑ablative fractional lasers) are added under dermatologist supervision. Strict photoprotection with a broad‑spectrum SPF 30+ (preferably tinted with iron oxides for visible‑light protection) applied every morning and reapplied throughout the day is essential to prevent relapse and to boost the efficacy of all topical agents.
Which creams are recommended for treating melasma?
The most effective prescription cream is hydroquinone 4 % (often part of a triple‑combo). Over‑the‑counter options such as azelaic acid 15 % or niacinamide 5 % are useful for milder disease or sensitive skin. Additional adjuncts—kojic acid, vitamin C serums, retinoid‑only creams—can be incorporated to support brightening and skin health. Ongoing sunscreen use and gentle skin‑care are critical to maintaining results and preventing new pigment formation.
Tailored Treatments for Darker Skin Types
Darker Skin (Fitzpatrick ‑VI) Adjustments
| Aspect | Recommendation | Rationale |
|---|---|---|
| Sun protection | Broad‑spectrum SPF 30‑50 tinted with iron oxides | Blocks UV + visible light, reduces white cast |
| Hydroquinone | 2‑4 % (lower end) | Minimize risk of exogenous ochronosis |
| Azelaic acid | 15‑20 % | Well‑tolerated, anti‑inflammatory |
| Tranexamic acid | 2‑5 % topical or 250‑500 mg oral BID | Addresses vascular component |
| Chemical peels | Glycolic 20‑30 % or salicylic 15‑20 % (superficial) | Gentle exfoliation, low PIH risk |
| Procedural | Microneedling + RF (Morpheus8) or non‑ablative 1064 nm Nd:YAG | Enhances drug delivery, targets dermal melanin |
| Maintenance | Daily sunscreen, avoid aggressive scrubs | Prevents post‑inflammatory hyperpigmentation |
 Managing melasma in Fitzpatrick III‑VI skin requires a regimen that balances efficacy with safety. First, photoprotection is non‑negotiable. Broad‑spectrum sunscreen with SPF 30‑50 that contains iron oxides (tinted formulas) blocks ultraviolet radiation and high‑energy visible light, the drivers of pigment in darker skin, and offers camouflage without a white cast, improving adherence.
Managing melasma in Fitzpatrick III‑VI skin requires a regimen that balances efficacy with safety. First, photoprotection is non‑negotiable. Broad‑spectrum sunscreen with SPF 30‑50 that contains iron oxides (tinted formulas) blocks ultraviolet radiation and high‑energy visible light, the drivers of pigment in darker skin, and offers camouflage without a white cast, improving adherence.
Topical therapy should start with low‑concentration hydroquinone (2‑4 %) combined with azelaic acid (15‑20 %). Hydroquinone inhibits tyrosinase, while azelaic acid provides anti‑inflammatory benefits and is well tolerated, reducing irritation and exogenous ochronosis. For patients who cannot use hydroquinone, azelaic acid alone or tranexamic acid may be substituted.
Procedural adjuncts safe for deeply pigmented skin include microneedling paired with radio‑frequency (e.g., Morpheus8) and non‑ablative fractional lasers such as 1064 nm Nd:YAG. These modalities enhance drug delivery and target dermal melanin with minimal thermal damage.
Which treatments are effective for hyperpigmentation in darker skin tones? For darker skin tones, the cornerstone of treatment is a broad‑spectrum sunscreen that blocks both UV and visible light to prevent new pigment formation. First‑line topicals include hydroquinone (often 4 % or lower), azelaic acid 15‑20 %, tranexamic acid, and low‑concentration chemical peels that reduce melanin production while minimizing irritation. Gentle chemical peels (glycolic acid or salicylic acid) can improve texture without triggering post‑inflammatory hyperpigmentation. Safe procedural options include microneedling with radio‑frequency and non‑ablative lasers such as fractional Nd:YAG 1064 nm, which target deeper pigment with low risk of adverse changes. A tailored regimen combining photoprotection, topical agents, and, when appropriate, in‑office procedures yields the most effective, sustainable results for hyperpigmentation in darker skin.
Procedural Interventions and Device‑Based Therapies
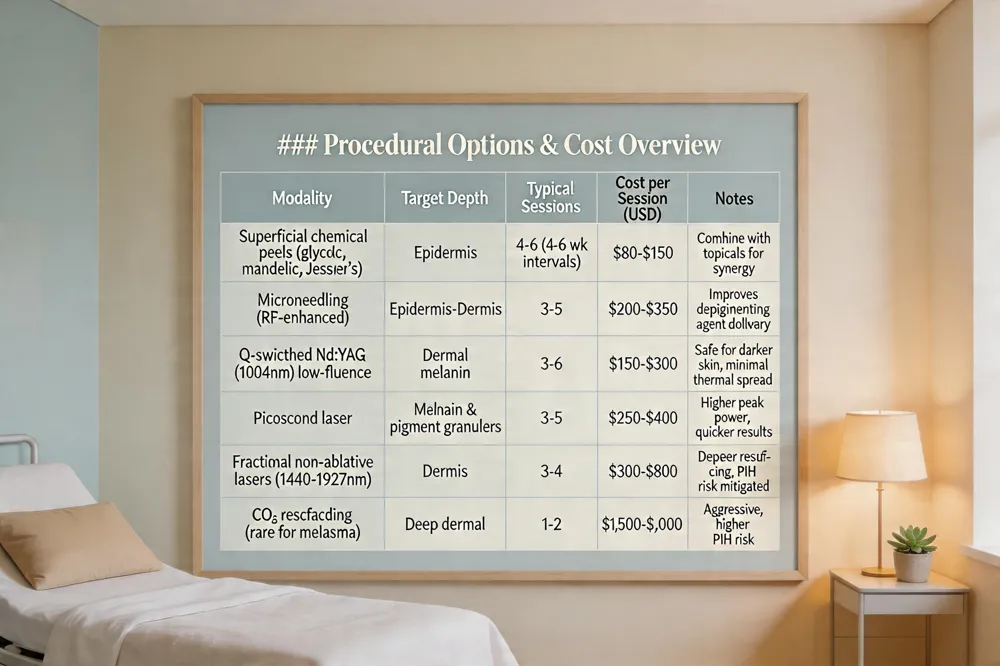
Procedural Options & Cost Overview
| Modality | Target Depth | Typical Sessions | Cost per Session (USD) | Notes |
|---|---|---|---|---|
| Superficial chemical peels (glycolic, mandelic, Jessner’s) | Epidermis | 4‑6 (4‑6 wk intervals) | $80‑$150 | Combine with topicals for synergy |
| Microneedling (RF‑enhanced) | Epidermis dermis | 3‑5 | $200‑$350 | Improves delivery of depigmenting agents |
| Q‑switched Nd:YAG (1064 nm) low Low‑fluence | Dermal melanin | 3‑6 | $150‑$300 | Safe for darker skin, minimal thermal spread |
| Picosecond laser | Melanin & pigment granules | 3‑5 | $250‑$400 | Higher peak power, quicker results |
| Fractional non‑ablative lasers (1440‑1927 nm) | Dermis | 3‑4 | $300‑$800 | Deeper resurfacing, risk of PIH mitigated with proper pre‑care |
| CO₂ resurfacing (rare for melasma) | Deep dermal | 1‑2 | $1,500‑$3,000 | Aggressive, higher PIH risk |
 Melasma treatment increasingly relies on procedural and device‑based options that complement topical regimens and strict photoprotection.
Melasma treatment increasingly relies on procedural and device‑based options that complement topical regimens and strict photoprotection.
Chemical peels and micro‑needling
Gentle superficial peels (glycolic, mandelic, Jessner’s solution) exfoliate the pigmented epidermis and promote uniform melanin clearance while minimizing irritation. When combined with topical agents such as azelaic acid, niacinamide, or hydroquinone alternatives, peels can accelerate improvement of epidermal and mixed melasma. microneedling creates micro‑channels that enhance trans‑dermal delivery of depigmenting creams, stimulating collagen remodeling and helping to even pigment distribution.
Laser options and cost considerations
Low‑fluence Q‑switched Nd:YAG (1064 nm) and picosecond lasers are the most studied for melasma, targeting melanin with minimal thermal spread. Fractional non‑ablative lasers (e.g., 1440‑1927 nm) offer deeper dermal resurfacing with a lower risk of post‑inflammatory hyperpigmentation. Typical pricing ranges from $150‑$300 per Q‑switched session and $300‑$800 per fractional session; 3‑6 treatments are usually required, bringing total costs to $450‑$2,500.
Morpheus8 usage and safety
Can Morpheus8 be used on patients with melasma? Yes, Morpheus8 (radio‑frequency microneedling) can be offered to patients with melasma, but it should be used with caution. The treatment’s controlled thermal injury can stimulate collagen remodeling and help even pigment distribution, especially when paired with topical depigmenting agents such as azelaic acid, niacinamide, or hydroquinone alternatives. Because any heat‑based procedure can provoke inflammation, broad‑spectrum sunscreen (SPF 30 or higher) and a consistent skincare regimen are essential to prevent worsening of the hyperpigmentation. Morpheus8 is typically considered an adjunct to standard melasma therapies rather than a first‑line option. A dermatologist should evaluate the patient’s skin type, melasma severity, and overall treatment plan before proceeding.
What are the most effective ways to remove facial pigmentation permanently?
Permanent reduction of facial pigmentation usually requires a combination of topical therapy, procedural treatment, and diligent sun protection. Prescription agents such as hydroquinone, retinoids, azelaic acid, or kojic acid can lighten existing spots and prevent new ones when used consistently. Periodic chemical peels (glycolic, trichloroacetic) and resurfacing procedures like microneedling help accelerate pigment turnover. Targeted laser or light‑based devices—particularly Q‑switched Nd:YAG, picosecond lasers, or fractional lasers—destroy melanin‑producing cells and often give the most lasting results. Finally, daily broad‑spectrum sunscreen (SPF 30 or higher) is essential to maintain improvements and avoid recurrence.
What is the typical cost of laser treatment for hyperpigmentation?
Laser treatment for hyperpigmentation typically costs between $150 and $300 per session for Q‑switched Nd:YAG lasers, which are often used to target pigment spots. Fractional non‑ablative lasers are a bit pricier, ranging from $300 to $800 per treatment session. Most patients need a series of 3–6 sessions to achieve optimal results, so the total out‑of‑pocket expense can fall anywhere from $450 to $2,500. For more aggressive options such as CO₂ resurfacing, costs can reach $1,500 to $3,000 per session, but this is less commonly used for simple hyperpigmentation.
Special Considerations: Periorbital Melasma
Periorbital Melasma Tips
| Recommendation | Details |
|---|---|
| Sunscreen | Mineral or tinted SPF 30+ applied every 2 hrs; choose fragrance‑free |
| n | Topicals |
| Antioxidant serums | Vitamin C 10‑15 % or niacinamide 5 % to boost protection |
| Procedural | Low‑fluence Q‑switched Nd:YAG, gentle glycolic/lactic peels, low‑setting microneedling |
| Follow‑up | Review every 4‑6 weeks to monitor irritation and pigment response |
 Periorbital melasma presents a unique challenge because the skin around the eyes is exceptionally thin and prone to irritation. The first line of defense is rigorous photoprotection: a broad‑spectrum SPF 30+ sunscreen—ideally a mineral or tinted formula containing iron oxides to block UV and visible light—should be applied daily and reapplied every two hours when outdoors.
Periorbital melasma presents a unique challenge because the skin around the eyes is exceptionally thin and prone to irritation. The first line of defense is rigorous photoprotection: a broad‑spectrum SPF 30+ sunscreen—ideally a mineral or tinted formula containing iron oxides to block UV and visible light—should be applied daily and reapplied every two hours when outdoors.
Gentle topical agents are preferred. Fifteen‑percent azelaic acid offers anti‑inflammatory and tyrosinase‑inhibiting effects with low irritation risk, while a low‑concentration hydroquinone (2 %) can be used short‑term under dermatologist supervision. Adding a vitamin C or niacinamide serum boosts antioxidant protection and helps even skin tone.
When topical therapy alone is insufficient, low‑risk procedural options can be considered. Superficial chemical peels using glycolic or lactic acid, microneedling with gentle settings, and low‑fluence Q‑switched Nd:YAG laser treatments target melanin while minimizing post‑inflammatory hyperpigmentation.
Regular follow‑up appointments allow the dermatologist to monitor response, adjust the regimen, and ensure the delicate eye area remains healthy throughout treatment.
Hyperpigmentation on the Body – Comprehensive Care
Body Hyperpigmentation Management
| Modality | Typical Use | Key Points |
|---|---|---|
| Prescription topical | Hydroquinone 4 % + retinoid or azelaic acid | Apply twice daily, monitor for irritation |
| Alternatives | Tranexamic acid, niacinamide, cysteamine | For hydroquinone‑intolerant patients |
| Chemical peels | Glycolic 20‑30 % or salicylic 15‑20 % (every 4‑6 weeks) | Enhances penetration, safe for Fitzpatrick III‑VI |
| Laser/IPL | Low‑energy Q‑switched Nd:YAG or IPL | Reserved for refractory lesions |
| Sun protection | Broad‑spectrum SPF 30‑50 with iron oxides | Essential for preventing new pigment |
 Body hyperpigmentation often involves large surface areas, so a treatment plan must combine efficacy with safety.
Body hyperpigmentation often involves large surface areas, so a treatment plan must combine efficacy with safety.
Topical regimens for large surface areas – First‑line therapy is a prescription‑strength topical regimen, most commonly hydroquinone 4 % paired with a retinoid or azelaic acid. Hydroquinone inhibits tyrosinase, reducing melanin synthesis, while the retinoid or azelaic acid promotes epidermal turnover and minimizes irritation. For patients who cannot tolerate hydroquinone, alternatives such as tranexamic acid, niacinamide, or cysteamine can be used. Consistent application twice daily and gentle moisturizers help maintain barrier integrity across extensive skin.
Chemical peels for body – Superficial peels (glycolic, lactic, or salicylic acid) exfoliate the stratum corneum, allowing deeper penetration of topical agents. When performed by a board‑certified dermatologist, spaced‑out peels (every 4–6 weeks) accelerate fading of epidermal pigment without causing post‑inflammatory hyperpigmentation, especially in Fitzpatrick III‑VI skin.
Laser and IPL for extensive lesions – Low‑energy Q‑switched Nd:YAG or intense pulsed light (IPL) can target melanin directly in stubborn or deeper dermal lesions. These modalities are best reserved for cases refractory to topical and peel therapy and require pre‑and‑post‑treatment skin preparation and gentle time‑energy risk need operators.
Answer to the key question – The most effective first‑line therapy for body hyperpigmentation is a prescription‑strength topical regimen, typically a combination of hydroquinone 4 % with a retinoid or azelaic acid to inhibit melanin production and promote cell turnover. Adjunctive chemical peels—such as glycolic, lactic, or salicylic acid—can deepen the effect by exfoliating the stratum corneum and allowing the topical agents to penetrate more uniformly across larger surface areas. For extensive or stubborn lesions, low‑energy laser or intense pulsed light (IPL) treatments target melanin directly and can accelerate fading while minimizing damage to surrounding tissue. Consistent broad‑spectrum sun protection (SPF 30 + with UVA/UVB and visible‑light filters) is essential to prevent new pigment formation and to maintain results. A personalized plan that integrates these modalities, monitored by a board‑certified dermatologist, yields the safest and most durable improvement for body hyperpigmentation.
Systemic, Lifestyle, and Maintenance Strategies
Systemic & Lifestyle Adjuncts
| Strategy | Dose/Regimen | Primary Benefit |
|---|---|---|
| Oral tranexamic acid | 250‑500 mg BID (2‑4 weeks) | Inhibits melanogenesis, reduces vascular component |
| Antioxidant diet | Vitamin C 500‑1,000 mg, Vitamin E 400 IU, polyphenol‑rich foods | Reduces ROS‑driven melanin synthesis |
| Supplements | Niacinamide 500 mg daily | Improves barrier, anti‑inflammatory |
| Sun avoidance | Wide‑brimmed hat, peak‑hour avoidance (10 am‑4 pm) | Decreases UV exposure |
| Consistent sunscreen | SPF 30+ with zinc/titanium oxide & iron oxides | Blocks UV + visible light, maintains remission |
| Trigger review | Hormonal meds, photosensitizing drugs | Discontinue or substitute when possible |
 Melasma is a chronic hyperpigmentation disorder that rarely disappears completely because its drivers—hormonal fluctuations, genetic predisposition, and UV/visible‑light exposure—remain present. The most reliable way to keep the condition in long‑term remission is rigorous broad‑spectrum sunscreen (SPF 30 + ) containing zinc oxide, titanium dioxide, and iron oxides should be applied every morning, reapplied every two hours, and used even on cloudy days or when indoors near windows.
Melasma is a chronic hyperpigmentation disorder that rarely disappears completely because its drivers—hormonal fluctuations, genetic predisposition, and UV/visible‑light exposure—remain present. The most reliable way to keep the condition in long‑term remission is rigorous broad‑spectrum sunscreen (SPF 30 + ) containing zinc oxide, titanium dioxide, and iron oxides should be applied every morning, reapplied every two hours, and used even on cloudy days or when indoors near windows.
Oral tranexamic acid (250–500 mg twice daily) has emerged as an effective systemic adjunct, especially for refractory or dermal melasma. It inhibits melanogenesis and reduces vascular contribution without the irritation associated with topical agents, though patients must be screened for clotting disorders.
Dietary antioxidants and supplements—vitamin C, vitamin E, polyphenols, and niacinamide‑rich foods—support skin health by neutralizing reactive oxygen species that amplify melanin production. While not a substitute for prescription therapy, a diet rich in fruits, vegetables, and whole grains can enhance overall treatment response.
Long‑term trigger avoidance includes wearing wide‑brimmed hats, avoiding peak UV hours (10 a.m.–4 p.m.), minimizing heat exposure, and reviewing hormonal medications with a physician.
Answers to common questions
- Can melasma be stopped permanently? Permanent cure is uncommon, but sustained remission is achievable with daily sunscreen, Kligman‑type triple‑combination creams, periodic procedural boosts (chemical peels, low‑dose Q‑switched laser), and consistent avoidance of known triggers.
- How can melasma be addressed from the inside out? Combine strict photoprotection, oral tranexamic acid, and an antioxidant‑rich diet to reduce melanocyte activation systemically.
- What natural methods can help treat melasma on the face? Gentle agents such as aloe vera gel, licorice extract (glabridin), and niacinamide moisturizers can modestly lighten patches when used alongside sunscreen.
- What is the fastest natural way to lighten melasma? Pair a mineral SPF 30+ sunscreen with a daily vitamin C/niacinamide serum and evening aloe vera or potato‑juice applications; visible improvement often appears within 4–6 weeks.
Putting It All Together – Dermatologist Guidance and Patient Expectations
Integrated Care Pathway
| Step | Action | Expected Timeline |
|---|---|---|
| 1. Assessment | Wood’s lamp/dermatoscope to determine pigment depth | Immediate |
| 2. Prescription | Triple‑combo cream (hydroquinone + tretinoin + low‑potency steroid) + SPF 30+ | Start day 1 |
| 3. Adjuncts | Add azelaic acid, tranexamic acid, or chemical peel if needed | 2‑4 weeks |
| 4. Procedural boost | Q‑switched Nd:YAG or microneedling for resistant areas | After 8‑12 weeks of topical response |
| 5. Maintenance | Daily sunscreen, intermittent hydroquinone/retinoid, lifestyle tweaks | Ongoing |
| 6. Expectations | 30‑70 % pigment reduction in 3‑12 months; lifelong sun protection to prevent relapse | 3‑12 months |
| 7. Cost overview | Q‑switched $150‑$300 per session, fractional $300‑$800; total $450‑$2,500 for typical series | Variable |
 When a patient walks into a dermatology office with melasma, the first step is a thorough visual exam, often supplemented by a Wood’s lamp or dermatoscope to determine pigment depth. The dermatologist will typically prescribe a prescription‑strength triple‑combination cream that pairs hydroquinone (a tyrosinase inhibitor) with a retinoid such as tretinoin and a mild corticosteroid. This regimen reduces melanin production, speeds epidermal turnover, and minimizes irritation. Broad‑spectrum sunscreen (SPF 30 or higher) with physical blockers like zinc oxide, titanium dioxide, and iron oxides is mandatory and must be reapplied every two hours, especially after swimming or sweating.
When a patient walks into a dermatology office with melasma, the first step is a thorough visual exam, often supplemented by a Wood’s lamp or dermatoscope to determine pigment depth. The dermatologist will typically prescribe a prescription‑strength triple‑combination cream that pairs hydroquinone (a tyrosinase inhibitor) with a retinoid such as tretinoin and a mild corticosteroid. This regimen reduces melanin production, speeds epidermal turnover, and minimizes irritation. Broad‑spectrum sunscreen (SPF 30 or higher) with physical blockers like zinc oxide, titanium dioxide, and iron oxides is mandatory and must be reapplied every two hours, especially after swimming or sweating.
If topical therapy alone is insufficient, adjunctive options are added. Gentle chemical peels (glycolic, mandelic, or Jessner’s solution) and microneedling enhance drug penetration, while low‑fluence Q‑switched Nd:YAG or picosecond lasers target deeper dermal pigment. Oral tranexamic acid may be considered for refractory cases after screening for clotting disorders.
Patients should expect a gradual improvement over 3‑12 months, with realistic goals of 30‑70 % pigment reduction. Maintenance involves lifelong sun protection, periodic reassessment, and possible intermittent resurf‑quinone or retinoid use to prevent relapse. Costs vary: Q‑switched laser sessions range $150‑$300 each, fractional non‑ablative lasers $300‑$800, typically requiring 3‑6 sessions. A personalized, stepwise approach balances efficacy, safety, and cost while setting clear expectations for long‑term skin health.
Sustaining Clear Skin – The Ongoing Commitment
In melasma management, lasting results depend on a three‑pronged strategy that blends vigilant photoprotection, targeted topical therapy, and occasional procedural interventions. Broad‑spectrum sunscreen—ideally SPF 30 or higher and tinted with iron oxides to block UVA, UVB and high‑energy visible light—should be applied every morning, reapplied every two hours, and complemented with wide‑brimmed hats and UPF‑rated clothing. Topical regimens often start with a triple‑combination cream (hydroquinone, tretinoin, and a mild corticosteroid) or, for sensitive skin, azelaic acid, niacinamide, or tranexamic acid, applied before sunscreen to maximize penetration. For patients with deeper dermal pigment, gentle chemical peels, microneedling, or low‑fluence Q‑switched lasers can accelerate clearance when performed by a board‑certified dermatologist. Regular follow‑up visits every 4–6 weeks allow the clinician to assess MASI scores, adjust agents, and monitor for side‑effects such as irritation or post‑inflammatory hyperpigmentation. Education empowers patients: understanding triggers like hormonal changes, heat, and blue‑light exposure, recognizing the need for consistent sunscreen re‑application, and learning how to use camouflage makeup after treatment creates a collaborative partnership that sustains a more even skin tone over the long term.
